
What is RCM and why are health systems in 2026 rushing to validate their revenue faster than ever? Learn how Al-assisted RCMs are transforming financial recovery timelines, cutting costs, and enabling even large enterprises to build compliance-ready pipelines in weeks.
Healthcare leaders are not asking whether Revenue Cycle Management works. They are asking whether it is sustainable. In the current economic climate, denial rates are rising, administrative costs are expanding faster than margins, and staffing shortages are slowing collections. Compliance complexity increases with every payer rule update, turning revenue leakage from a billing inefficiency into a board-level strategic risk.
The financial pressure on providers has reached a tipping point. While historical averages were lower, current data reveals that more than 41% of healthcare providers now face denial rates higher than 10%. Furthermore, although 60% of denied claims are eventually resubmitted, only about two-thirds of those resubmissions are successfully overturned, leaving a massive portion of revenue permanently unrecovered. This makes the revenue cycle a primary concern for the C-suite. Hospitals now spend approximately 15-30% of their total expenditures on administrative and operational costs, a figure that continues to climb as payer requirements become more fragmented. Meanwhile, Al-driven operational models in adjacent industries are reducing costs by double-digit percentages. The question is no longer whether to automate; the question is whether your Revenue Cycle Management is intelligent. Al in Revenue Cycle Management represents a shift from rule- based processing to predictive, adaptive, and continuously learning revenue intelligence systems.
What Is Revenue Cycle Management in Healthcare?
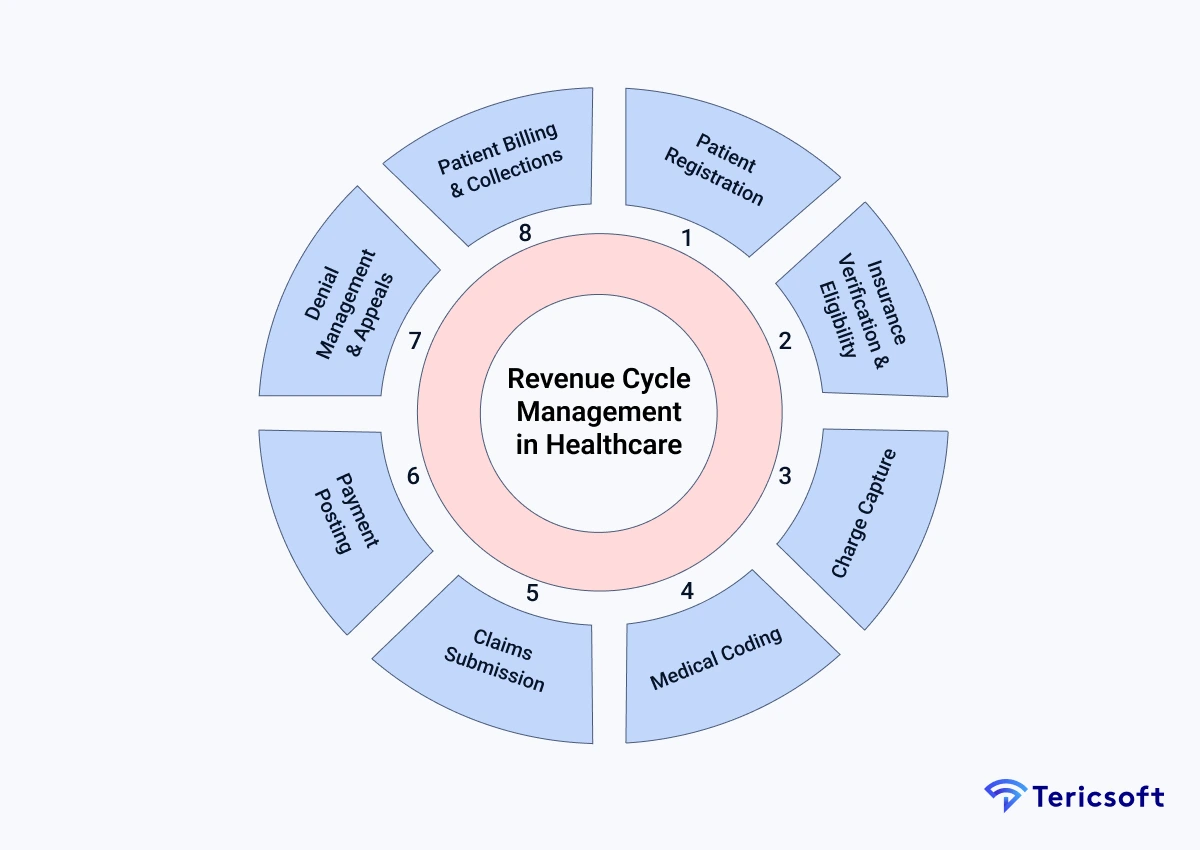
Revenue Cycle Management (RCM) in healthcare governs the financial lifecycle of patient care, spanning from the moment a patient schedules an appointment to the final payment of the balance. It is the backbone of the healthcare provider's financial health, ensuring that clinical services are translated into sustainable revenue.
RCM Meaning
RCM meaning refers to the structured financial process that uses billing software and clinical documentation to ensure healthcare providers are compensated accurately and efficiently for their services. It encompasses the entire front-end patient interaction and back-end billing and collections.
Key Stages of the Revenue Cycle
The complexity of RCM requires a meticulous approach at every touchpoint. The following table outlines the critical phases where intelligence can be applied to maximize yield.
Revenue Cycle Management Is Critical
Revenue Cycle Management is critical because it determines hospital cash flow stability and directly impacts EBITDA margins. Beyond the balance sheet, it influences patient satisfaction through billing transparency and affects long-term financial resilience. A broken RCM process leads to bad debt and administrative burnout, whereas an optimized one provides the capital necessary for clinical innovation and expanded patient services.
What Is Al in Revenue Cycle Management?
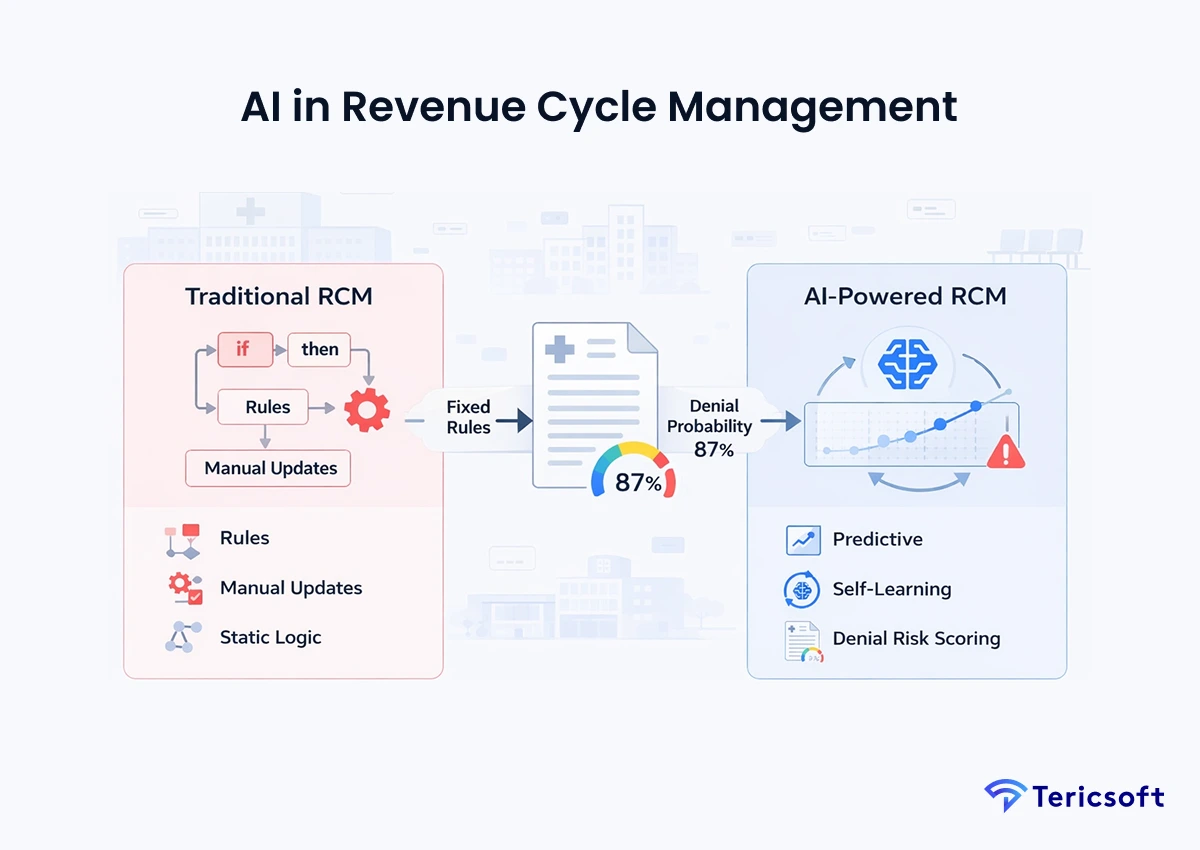
Al in Revenue Cycle Management integrates machine learning (ML), predictive analytics and natural language processing (NLP) into existing RCM workflows. While traditional RCM relies on static, "if-then" logic, Al-driven RCM utilizes dynamic models that improve over time by analyzing historical data.
Traditional Automation vs Al Intelligence
Traditional RCM automates tasks based on fixed rules. If a payer changes a rule, a human must manually update the system. In contrast, Al in Revenue Cycle Management predicts outcomes. It can look at a claim and determine the statistical likelihood of a denial based on thousands of previous interactions, even if the specific rule has not been hard-coded into the system yet.
Why Al Is Becoming Essential in Modern RCM
The modern healthcare landscape is characterized by increasing payer complexity and rapid rule changes. According to the Experian Health 2025 State of Claims survey, 41% of providers now face denial rates of 10% or higher, highlighting a systemic challenge that manual processes can no longer solve. Staffing shortages have also left many billing departments under-resourced. Al enables systems to learn from patterns instead of relying on static rules, allowing organizations to scale their financial operations without a linear increase in headcount.
"Automation and machine learning promise to revolutionize revenue cycle management by automating routine tasks, addressing staffing shortages, and swiftly adapting to changes. The technology's trajectory demands leaders' attention to harness its potential effectively."
— Seth Katz, Vice President of HIM and Revenue Cycle at University Health KC
How Al Is Used in RCM?
Al is embedded across core Revenue Cycle Management workflows to eliminate friction and maximize yield. This integration allows for a seamless transition between clinical documentation and financial reimbursement.
Al in Medical Billing and Coding
Al in medical billing and coding improves coding accuracy, reduces compliance risk, and minimizes human error in ICD and CPT assignments. By using Natural Language Processing (NLP), Al can read through unstructured clinical notes and suggest the most appropriate codes, ensuring that the documentation supports the level of care provided.
"Our Al, understanding clinical language, accelerates coding, improves accuracy, and cuts costs. I'm excited about Al's future impact in RCM."
— Anne Robertucci, Vice President at Prisma Health
Al for Claims Processing
Al for claims processing predicts denial risk before submission. Al-enabled platforms have demonstrated the ability to achieve significantly higher first-pass clean claim rates, effectively eliminating the need for manual verification in the vast majority of transactions. This first-pass optimization ensures that claims meet the specific requirements of different insurance carriers.
Al in Patient Eligibility
Al in patient eligibility automates coverage validation and identifies missing authorizations. Front-end revenue leakage often occurs because a patient's insurance changed or a specific procedure required prior authorization that was not obtained. Al monitors these status changes continuously, alerting staff to discrepancies before the patient arrives.
Al for Denial Management
Instead of just helping staff work through a list of denied claims, Al analyzes historical denial patterns to identify root causes. This intelligence turns the denial management office into a center for continuous process improvement.
"Al will transform RCM by automating tasks, reducing staff, cutting costs, and improving outcomes. It's streamlining workflows like authorization, payment processing, and claims adjudication."
— Todd Craghead, Vice President of Finance and Revenue Cycle at Intermountain Health
Al vs Traditional Revenue Cycle Management Systems
For executive evaluation, it is helpful to view the technological leap through a comparative lens. The transition from legacy systems represents a move from manual labor to cognitive computing.
Al does not replace Revenue Cycle Management systems; it transforms them into intelligent financial infrastructure that supports the entire enterprise.
Benefits of Al in Revenue Cycle Management
The implementation of Al offers quantifiable improvements across the entire financial spectrum of a healthcare enterprise, providing a clear return on investment.
- Reduced Denial Rates: 83% of healthcare organizations using Al report at least a 10% drop in denial rates within the first six months of implementation.
- Faster Revenue Realization: By increasing the clean claim rate, organizations reduce Days in Accounts Receivable (DAR), which directly improves liquidity and cash flow.
- Lower Administrative Burden: Organizations embedding Al within core billing workflows have achieved reductions in overall medical administrative spend of approximately 9% through accelerated automation and Al adoption.
- Enhanced Compliance Visibility: Explainable Al supports audit trails and regulatory oversight, providing a clear rationale for every coding decision.
Challenges of Implementing Al in Revenue Cycle Management
While the benefits are clear, the path to implementation requires strategic navigation. Success is found in the balance between technology and organizational governance.
Al adoption fails when governance is an afterthought. Successful enterprises prioritize a governance-first approach to ensure data integrity while fostering a culture of innovation.
The Future of Al in Revenue Cycle Management
Al will redefine Revenue Cycle Management from a transactional function into a predictive financial command center. Future RCM systems will forecast revenue risk in real-time, simulate payer behavior scenarios, and provide CFO-level dashboards that inform broader health system strategy.
In the next decade, Revenue Cycle Management will not be measured by collection speed but by predictive accuracy. The competitive advantage in healthcare finance will belong to organizations whose revenue cycle learns faster than their peers. Al in Revenue Cycle Management will become a margin defense strategy and not just an efficiency tool. As the industry moves toward value-based care, having a predictive financial engine will be the differentiator between thriving and merely surviving.
How Tericsoft Enables Enterprise Al in Revenue Cycle Management
Tericsoft does not replace Revenue Cycle Management systems. Instead, Tericsoft acts as an Al intelligence and governance layer that enhances existing RCM infrastructure. We focus on the Intelligence Layer, providing advanced analytics that transform raw RCM data into predictive revenue insights.
Our architecture is Governance-First, ensuring that all Al applications are compliance-ready and aligned with HIPAA and enterprise audit standards. Through our secure integration model, we work alongside EHR platforms, billing systems, and payer interfaces without causing operational disruption. We help enterprises make their Revenue Cycle Management smarter without requiring them to rebuild it from scratch.
About Tericsoft
Tericsoft designs compliance-first Al intelligence systems for regulated enterprises. We specialize in enterprise Al strategy, compliance-driven infrastructure, and scalable intelligence frameworks for healthcare finance.
AI in Revenue Cycle Management uses machine learning and predictive analytics to reduce claim denials, improve billing accuracy, and optimize healthcare cash flow.
AI analyzes historical payer data to predict denial risks before submission, enabling proactive corrections and higher first pass clean claim rates.
Yes, enterprise AI in RCM can be built with governance frameworks, encryption, audit trails, and explainable models to ensure HIPAA compliance.
AI improves coding accuracy, reduces administrative workload, accelerates reimbursements, and minimizes compliance risks.
No, AI typically acts as an intelligence layer that enhances existing RCM infrastructure rather than replacing core billing systems.








